Welcome to the final part of our second birth story – which has been sat in my drafts for a good 12+ months! Despite a textbook fast and spontaneous labour the first time around, this baby was in far less of a hurry to come out. If you’ve not read part one, you can find it here and part two here. Otherwise, if you’re all up to date, you’ll find us making our way on to labour ward after a failed induction.
When we arrived at the hospital, it was 12pm… bang on Sunday lunch time. Having had the pessary inserted and my waters breaking just a few hours later, we were sure that we’d be a family of four by that evening. Our smugness at the fast progression was short-lived, thirty three hours after arriving at the hospital we still had no baby and were off to labour ward for a drip induction.
I was nervous, so incredibly nervous as the midwife took us through. From the word go, I’d wanted to avoid being induced via drip. I’d refused to read up on it and had only really heard horror stories of long, intense labours and being stuck on a bed. In our hospital the midwife led unit, ante and post-natal care wards are just across the corridor from the labour ward meaning a short walk out of the main unit and into our new room. ‘You won’t leave this room until you’ve had your baby’, the midwife said as we pushed open the door. Gulp!
Inside the room was far less clinical than I was expecting. The bed was a birthing bed designed to have bits added and removed to suit a labouring woman’s whim, alongside was a birthing stool, a yoga ball and mats should I wish to get down on the floor. Monitors were tucked discretely in the corner and a baby resuscitation/care cot was behind a curtain incase it was needed. A bathroom (shared with next door) and chairs were on the other side but most importantly, it had air con! So far in this birth it had been hot, ridiculously hot, and the rooms on the ward were stifling. It was actually part of how they got me through into the labour ward so easily – anything to be cool!
We popped our stuff down, had a wee and sent a message to our family to say things were a go. First up, monitors on. Thankfully labour ward had wireless monitors meaning one less thing to be attached to. Not only that but they could monitor them from the main desk if I wanted, meaning we could be alone in the room throughout – I could even have the screen turned off. With one monitor for me and one for the baby, it was time to hop up on the bed for what I can honestly say was the worst bit… the cannula.
I have a massive hatred of blood being taken or thinking about my veins so I’m not lying when I say that the cannula was the bit I really didn’t want to see. I’m right handed so they offered to put it into my left hand in the hope that it would be less in the way, I didn’t care, I just wanted it covered! Thankfully the midwife was incredibly accommodating of this and covered it in a bit of bandage and tape to make it as unobtrusive as possible. Cannula in, monitors on, baby happy, it was time to move on with induction.
At this point the midwife explained what would happen. They’d check my waters had gone and if they hadn’t, they’d artificially break them in order to bring labour on. Next, they’d hook up the hormone drip in order to bring on labour. They’d start with a teeny, tiny amount, keep it at that rate of flow for thirty minutes and then double the dosage, wait another thirty minutes and double it again. This would continue until they were happy that I was in active labour. Throughout both me and the baby would be monitored to make sure we didn’t go into hyper-drive and get stressed. Once in active labour, they’d stop doubling the drug and things would progress at my body’s own speed.
With that in mind, I had yet another examination. They quickly realised that my waters hadn’t actually gone, believing instead that it was a hind water leak; the bag of waters had a hole in it, leaked and the baby’s head had dropped down and plugged the leak itself. So first on the list of delights was an artificial rupturing of membranes; aka. the midwife with a big hook. She warned me it would be uncomfortable and she wasn’t lying. Like an incredibly vicious sweep, there was a fair amount of moving around as she did her best to break them. They did offer gas and air at this point but a bit of hand squeezing and some toe-curling got me through it; one bit done, all waters were now officially broken!
After that, they hooked up the drip to my cannula and we were ready to go, with all of the jobs done it was now just a case of letting the drip do it’s magic and wait for my body to kick into gear. We’d been in the room about 90 minutes, it was just after 10.35pm and we were back to the waiting game. My midwifery team consisted of two ladies; the main midwife and a student (a mum of four herself!) and we sat chatting to them happily whilst we waited. One of them suggested a TENS machine and helped me set that up; not that I needed it, I couldn’t feel a thing at this point!
About thirty minutes later they turned up the drip and contractions started to slowly creep in. We were chatting about midwifery training and TV shows when they noted that I was started to rock a little on the medicine ball as we spoke. Nothing really notable but some slight twinges close to period pains were coming… if it hadn’t been for the monitor, I think I’d have happily sat through them and dismissed them.
Again the drip was turned up and at around 11.30 they left the room to grab a drink. Over the last thirty minutes the contractions had become progressively stronger but still nothing that I couldn’t talk through. I thought I’d want to labour with just Dave and I but the distraction of conversation was lovely. When they left I realised that things were actually moving fairly quickly and I jumped off the ball to try an all-fours position on the floor. That brought no relief and with the majority of discomfort coming into my back I tried swaying against Dave for a while to no avail.
Just after twelve the midwives came back into the room and suggested trying to get up on the bed in order to lean over the back. I’d laboured on my knees the first time around and found it the most comfortable way so it seemed like a good idea to give it another try. Around now was when they agreed that I was in active labour; there was no need for the drip to continue as things were well and truly on their way!
With my arms over the back of the bed, I started breathing through the rather fast and strong contractions. They say that induced labour is harder because of the intensity of contractions but I can genuinely say it felt no different to the first time around. My first labour came on quickly, jumping straight into strong, long contractions and this one was exactly the same. Time seems to go differently when you’re in labour and I remember very little of this stage except concentrating on the TENS machine and getting a little tangled in my wires! In the background, I hear my midwife ask the student midwife if she’d ever delivered a baby in this position; she hadn’t and they chatted briefly about how to do it as I groaned away!
Suddenly everything changed and I needed to push. It felt like it had barely been minutes since they’d come back in the room! As the pressure to push came, I knew it was time for gas and air – I can’t believe I’d lasted that long without it. Whilst the pain reduction element was pretty tempting, I knew that it would help me focus my breathing more, as well as giving me something to bite down on when pushing. I remembered that from the first time! Last time Dave managed to wrestle the mouthpiece away from me between pushes but this time I was having none of it, from the moment I asked for it I wasn’t letting go! As I pushed, they got the baby bed ready just in case; something I both recognised and didn’t recognise at the time, when you’re in the zone, you’re in the zone!
That’s when things started to get a little more scary. After a few pushes, the midwife told me I had to get onto my back. Immediately I didn’t want to, all I could think of was how giving birth on your back is the hardest and least effective method to naturally help your baby out. The midwife wasn’t asking though, I had to get on my back immediately as they were losing the baby’s heart rate. Baby was progressing quickly down the birth canal and each time they moved, the monitors lost the heart rate. With the speed of delivery they were concerned about additional stress on the heart and needed to try and get a reading.
Into the room came the on call doctor for Obs and Gynae; aka ‘Lovely George’ (their name for him, not mine!). They wanted to try and pop a clip on baby’s head but were unable to get it to stay on so were keen that he was there just in case. Baby was getting increasingly stressed with the speed of delivery but wasn’t quite progressing. Looking back, we knew it was a little more serious when the student midwife was no longer leading my care but stood quietly in the corner out of the way. Instead, my main midwife was doing another check; they found the cause of the problem; a cervical lip.
Put simply, my cervix wasn’t quite dilated and as I pushed each time, baby’s head was banging on my cervix unable to progress and causing stress. This is where the fun began. My midwife asked me to trust her and do exactly what she said; with that we flipped my right leg up on to the left stirrup turning me onto my left side. Then my left leg onto my right stirrup flipping me back onto my other side. Anything to try and move the baby’s head slightly and encourage them to come down in a better position allowing my cervix to dilate fully. Finally, back on my back with both legs up, my midwife asked me not to push.
Have you ever tried that? When your body instinctively wants to do something with all it’s might but you can’t. She placed her head centimetres from mine and stared me in the eyes, ‘breathe’ she kept saying as we breathed through and didn’t push. In that moment there was no-one else in the room as far as I was concerned. I didn’t even know where Dave was – it was literally just me and her, getting through this. Still the cervical lip continued to remain a problem. There was one last thing for it, she was going to hold my cervix open and manually ‘reduce’ it.
Yep. You heard that right.
‘This is going to hurt but you can do it’ she said. In went her hand to hold open my cervix whilst I pushed with all my might. A big push later and we were past it; cervical lip rather painfully dealt with! As she moved out of the way, I looked up to find a room full of people; my two midwives, an additional one required for the birth (you have to have two qualified midwives for each birth), lovely George the doctor, a paediatric doctor and a paediatric nurse; all stood between my legs waiting for this baby to get the hell out.
Oh and Dave. Stood up the business end rather terrified.
With the baby now nearly out it was time for some big pushes or face an episiotomy or c-section due to the baby’s distress; one big push (and a poo!) followed by a short break to catch my breath. I remember turning my head to the side and just panting a little, feeling tired by all the action – I think if I could have, I’d have had a little nap! Another big push and the head was born.
That’s when we found out the real issue. Somehow, the baby had managed to get their umbilical cord wrapped around their neck and with each push this was pulling tighter. They quickly looped it back over and with a small push from me my baby was born!
‘I need to cut the cord, David, ok?’ said the midwife, cutting the cord and whipping the baby up on to my stomach. There was no noise, no movement and a very still, blue baby who suddenly was no longer on my lap. ‘Make my baby breathe’ I kept saying over and over as the doctor moved them over to the resuscitation bed explaining that they were breathing but needed a little help. With that a little cry came out! In the minutes that passed, I had the injection, birthed the placenta and got a severe case of the shakes (again! Apparently it’s my post-birth thing!).
‘What did we have?’ I asked Dave. He didn’t know. We both looked at the midwife, she didn’t know. ‘Shall I take a look?’ the paeds doctor said.
‘It’s a girl’
A girl.
Dave burst in to tears whilst I lay there in shock, tired and shaky. They placed her on my chest for the first time and she stared up with a decidedly grumpy looking face. We agreed her name would be fine and thanked the medical team. Phew, what a time!
Things then took another turn. Having left the room post birth, the Paeds team were suddenly back. They test bloods from the umbilical cord post birth and whilst the blood flow to her had been fine, the blood flow back was very low in oxygen meaning she’d been having to work very hard in the womb. This meant there was a significant risk of brain injury and she’d need monitoring on the Neo-Natal Unit. As the doctor explained this, it barely sunk in, I asked when they needed to take her. ‘Right now’ was the answer.
With that the Paeds team, extra midwife, student midwife and my baby left the room. I sent Dave with them, terrified that something would go wrong and she’d be on her own. It was just me and my midwife left. I’d managed to get through labour with just a small second degree tear (the exact same place as last time) and needed stitching before I could go with them. That was the strangest part of the whole thing; less than thirty minutes after giving birth I was on my own in the labour room, legs shaking like crazy and suck on the bed. My midwife had gone to get the suture kit, everyone else was with the baby and my phone and drink were just out of reach. It felt like I’d imagined the whole thing; had I really just given birth?!
The student midwife returned assuring me that everything was fine and they were settling in to the NICU. The midwife did the stitches, talking through it as she went. I forgot how painful the stitching can be; it was far more painful than the labour itself I think! Legs still shaking, they made me a cup of tea and forced me to have a shower. I couldn’t wait to get to the NICU but they both gave the same advice; shower now, just incase I wouldn’t get a chance later.
Once clean and dressed, they got a wheelchair and insisted on wheeling me down the corridor to the NICU. I arrived to a baby hooked up on cables with tiny needles into her scalp. Dave was sat in a chair holding her and looked terrified to move. It was horrible. From giving birth to coming back with her it had been about an hour and they’d had to give her sugar drops as she was hungry. They encouraged me to feed her but I was too scared to try and lift her out so the nurses helped get her into position; all those cables and monitors are incredibly off putting!
She latched on in seconds for her first feed; what a pro. Dave and I sat in the darkness listening to the beeps and quietly chatting. They needed to monitor her for seven hours after her birth to check on brain activity and ensure she didn’t have any seizures. If she passed this then there was likely to be no damage from the birth although they couldn’t guarantee there wouldn’t be an issue from earlier in my pregnancy if she’d gotten wrapped in the cord.
After 90 minutes or so, they sent me off to bed. It was 4.30am and leaving them sat with beeping monitors was one of the hardest things to do. We talked about telling family, I was keen to but Dave wanted to wait until we knew the outcome of the tests; why wake them to tell them when we wouldn’t yet have answers.
I managed an hour or so before waking again and making my way back to the NICU. Things had gone well in the night and they were happy that we could move off of the ward and back to the postnatal team. What a relief! By 9 we were on a normal ward, baby next to us and ready to contact our loved ones to share her arrival. What a journey!
Having had such a textbook labour the first time, I can honestly say that this one was such an emotional rollercoaster. From sitting around waiting to the fast labour and the stay on the NICU, I couldn’t get my head around what had happened and we were desperate to get home. Due to my waters breaking we needed to stay in for a further 24 hours, taking our hospital stay to 72 hours! Out of that time, I was in labour for 38 minutes, pushing for 17 minutes and the placenta came out 15 minutes later… talk about keeping us on our toes. I have a feeling that she’ll be doing that for years to come.
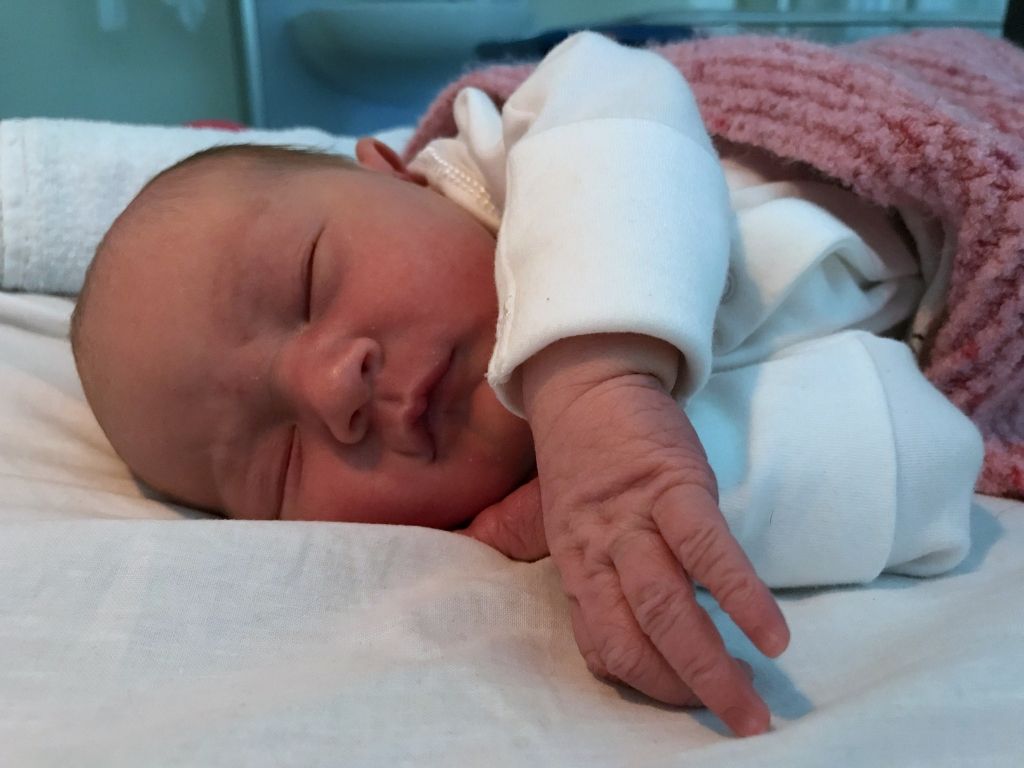
Welcome to the world baby girl.
8lb 15oz of perfection born at 12.55am; two years, three weeks and two minutes exactly after we started this parenting journey we were now parents of two!
Fancy another birth story? Read our quick first birth story here.









1 Comment
Oh my goodness! You told me about the cord at the time… But I had no idea about the rest! You must have gone through a rollercoaster of emotions and probably went through them all again when you wrote it down! Cord is scary enough on it’s own. I’m shaking reading this!